COVID-19 RESPONSE AND MAINTENANCE OF ESSENTIAL HEALTH SERVICES IN COSTA RICA
CONTENTS
QUICK DOWNLOADS

KEY INSIGHTS
Between March 2020 and December 2021, Costa Rica’s integrated health system enabled a rapid, coordinated response that may have limited the transmission of COVID-19 and helped avoid hospital saturation for most of the pandemic period. One of the most important aspects of the response was the Costa Rican Social Security Fund (Caja Costarricense de Seguro Social, CCSS), also known as CAJA, which took key actions aimed at mitigating the effects of the COVID-19 pandemic on the delivery of routine and essential health services.
This research has been led by partners at the INCAE Business School in collaboration with Brown University School of Public Health and Johns Hopkins Bloomberg School of Public Health and was supported and funded by The Rockefeller Foundation and by Gates Ventures.
Drivers of successful pandemic response
The World Health Organization and Global Health Security Agenda have developed useful frameworks for assessing epidemic and pandemic preparedness and response, which we have adapted for this research. Through our research, we aim to derive lessons learned about the drivers of a successful response and have developed a conceptual framework that categorizes the drivers into two groups: context and system factors and interventions, and also includes outcomes. The following pages on the Costa Rica’s response to COVID-19 and the maintenance of essential health services are organized according to this framework.
What were the most important elements of Costa Rica’s COVID-19 response?
There are many challenges with conducting research during an evolving pandemic, including quality of data and availability of interviewees involved in the response. In the absence of true impact measurements, we used alternative metrics as proxy indicators and developed criteria to help identify best practices, including overall reach and access, repeated mentions in key informant interviews, innovative or adaptive responses, potential for scale and impact, and equity considerations. Additionally, Costa Rica’s 2022 cyberattack created additional difficulty in accessing data throughout the research process.
System factors: health system strength and structure
Coordinating the response to COVID-19 prevention and essential health services maintenance
Costa Rica’s health system works from the top down as a single cohesive unit, enabling a coordinated response to the COVID-19 pandemic and the continued delivery of essential health services nationwide in the pandemic context.
Even before the COVID-19 pandemic began, CCSS’s integrated approach to health service delivery enabled system-wide decision-making and resource allocation, such as the need-based distribution of clinic supplies and strategic patient transfers to ease overload within the hospital network. Between March 2020 and December 2021, this strategy enabled real-time decisions about health policy and care delivery. For example, the Operational Coordination Council (Consejo de Coordinación de Operaciones), a group of health facility directors and other administrators in the public health sector, typically assesses needs, coordinates resources and patient movements, and prioritizes care according to demand. During the COVID-19 pandemic, the council met weekly instead of monthly and made critical system-wide decisions in response to urgent health system needs.

System factors: pandemic preparedness capacity
Using comprehensive, high-quality data to make informed decisions about COVID-19 prevention and treatment and essential health services maintenance

Costa Rica leveraged two preexisting data systems, the National Health Surveillance System (Sistema Nacional de Vigilancia Epidemiológica, SIVEI) and the Single Digital Health Record (Expediente Digital Único en Salud, EDUS) system for digital health records, to help identify COVID-19 cases, track the pandemic’s evolution in real time, and facilitate informed decision-making. SIVEI data helped shape and support contact tracing and testing strategies devised by the National Situation Analysis Room of the multidisciplinary Emergency Operations Center. EDUS data helped the CCSS allocate resources and distribute patients within the health system.
Decision-makers across CCSS were able to review EDUS data—including real-time information from all levels of the health system, such as daily reports of available and occupied intensive care units (ICU) beds—to identify and adjust the burden of demand on particular hospitals or health facilities. EDUS likewise contributed to the maintenance of essential health services during the COVID-19 pandemic by enabling easy access to medical records and communication between hospitals and health centers.
The cyber-attack that later occurred in May 2022 has underscored the importance of this system, and at the same time, it has pointed to the vulnerabilities that need to be addressed to ensure its survival.
Health system-level response measures
Streamlining bureaucracy for emergency response
The structure of Costa Rica’s health system predates the COVID-19 pandemic, and in the face of the health emergency the structure could be adapted quickly in March and April 2020—including by adjusting protocols for health personnel, expanding hospital capacity and infrastructure, and adapting virtual service modalities to maintain essential health services.
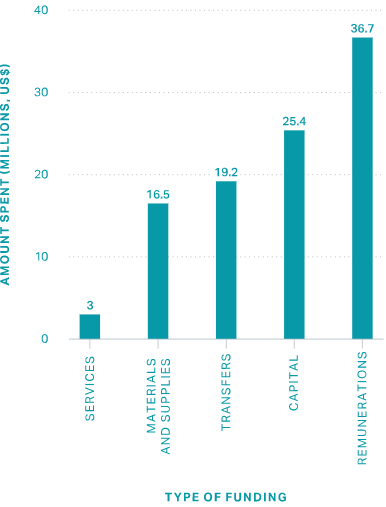
Likewise, a preexisting CCSS contingency fund made it possible to pay for rapid interventions, including a specialized COVID-19 treatment center (CEACO), an increased health workforce, and personal protective equipment (PPE) and other key supplies, as they were necessary.
National, governmental, and population-level measures: social distancing and mobility restrictions
Imposing stringent public health and social measures to delay the spread of COVID-19

In March 2020, Costa Rica’s Ministry of Health quickly acted to contain the spread of COVID-19. On March 16, the country’s president declared a State of National Emergency, which enabled the Ministry of Health to implement public health and social measures, including mobility restrictions and social distancing requirements, nationwide. Controlling the spread of COVID-19 freed up health system bandwidth and enabled the maintenance of essential health services.
National, governmental, and population-level measures: vaccination for pandemic pathogen
Acting early to secure vaccine doses
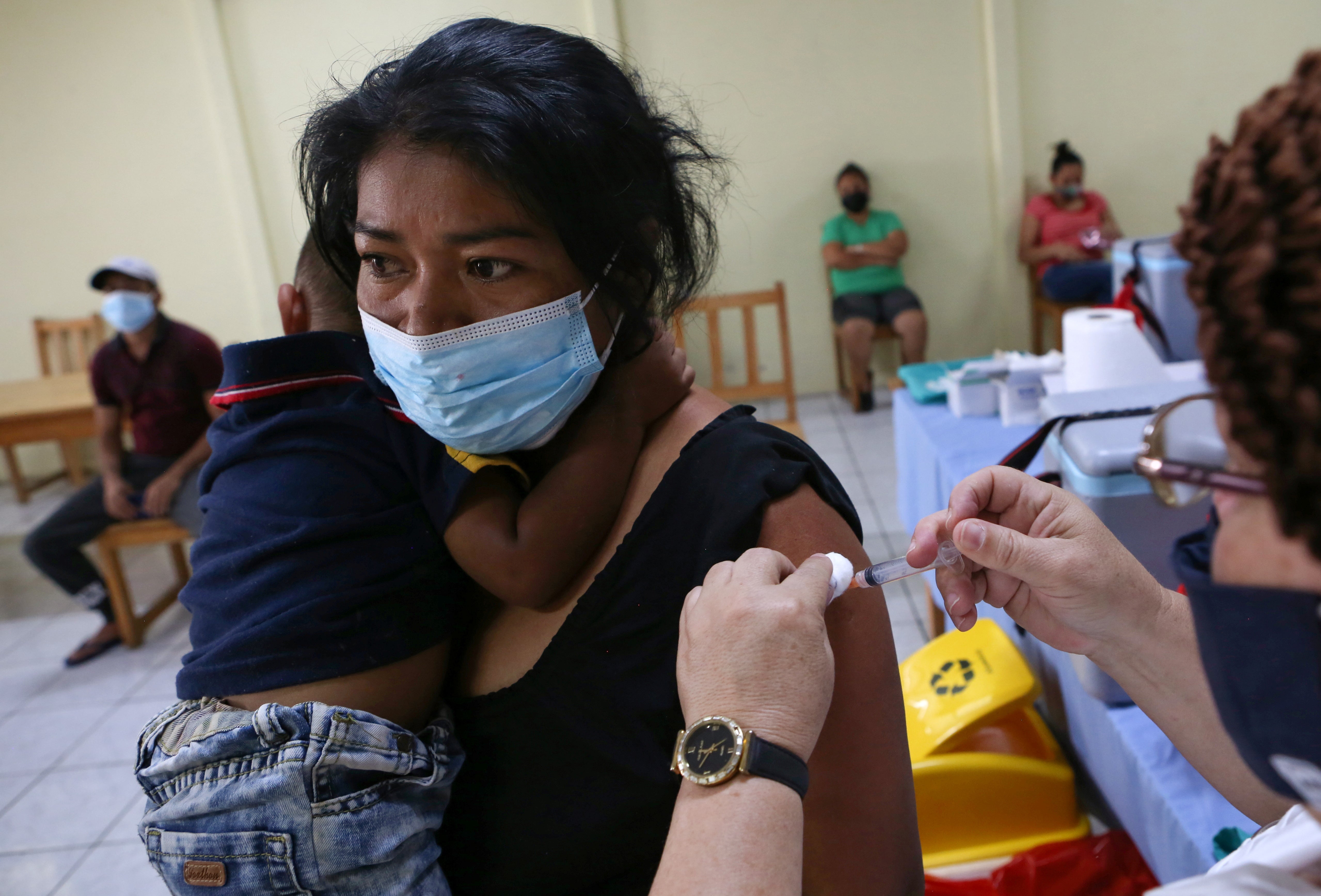
Costa Rica was one of the first Latin American countries to launch a COVID-19 vaccination campaign and achieve broad vaccine coverage for those willing to be vaccinated. They were especially able to garner support from entities like the Pan American Health Organization and the World Bank. Its vaccination campaign started with frontline health workers, which enabled a quicker return to in-person delivery of key essential health services. This broad vaccine coverage also likely slowed the spread of COVID-19.
Health system-level response measures: service delivery adaptation
Innovating for COVID-19 response and essential health services maintenance
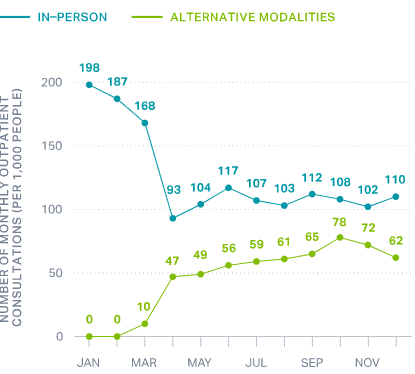
By the end of 2020, approximately 4,800 health workers in Costa Rica were delivering services remotely. (Key services, such as cardiology, oncology, COVID-19 diagnostics and treatment, and emergency care were delivered in person throughout the pandemic.) Using the EDUS data system, physicians working remotely could still access the tools they needed to care for patients and perform administrative tasks. For example, they could electronically review notes from previous medical appointments.
These health professionals provided online and telemedicine outpatient consultations and monitored asymptomatic COVID-19 patients by phone, keeping them out of hospitals and health facilities. The telemedicine they provided helped those facilities avoid saturation during pandemic waves.
COVID-19 RESPONSE AND MAINTENANCE OF ESSENTIAL HEALTH SERVICES IN COSTA RICA

Ask an Expert
Our team and partners are available to answer questions that clarify our research, insights, methodology, and conclusions.
