Key Points
Liberia developed a national, centralized monitoring and evaluation system that used CHWs in the field to serve as frontline data collectors.
Liberia developed and utilized detailed financial planning tools to guide conversations with donors.
Liberia harnessed partners’ resources to aid and expedite implementation and ongoing program management.
Over less than five years, Liberia, one of the poorest countries in the world, designed, piloted, improved, and launched a professionalized community health worker program that incorporates many key international best practices and serves 70 percent of the rural population while only adding five percent to the national health budget. A few key strategies allowed Liberia to quickly launch and sustain this robust community health worker program. These strategies include: strong government leadership in support of a well-articulated vision; a detailed financial plan and understanding of how donors could support that plan; and partners ready to support as needed. We will discuss each of these strategies in this section, in addition to the data systems and targeting that have helped provide windows into the program’s impact and support continuous improvements to maximize impact.
Political will

Generating political will and securing political commitment require excellent timing. Decision makers, for example, tend to be more open to new ideas and approaches during major political transitions and crises.
Liberia’s experience establishing the national CHW program in the wake of the Ebola crisis demonstrates the value of timing in politics. Supporters of CHW programming in Liberia recognized the Ebola epidemic had left government officials and their partners eager for sweeping reforms.
To leverage this opportunity, CHW supporters within and outside Liberia’s Ministry of Health acted swiftly. In 2013, as Deputy Health Minister, Dr. Bernice Dahn pushed for a roadmap toward a new community health system. During and post Ebola, as minister of health, Dr. Dahn worked with partners outside the MOH to highlight the opportunity to the president who, in December 2014, announced a commitment to making CHWs central to Ebola recovery.
In December 2014, Liberian President Ellen Johnson Sirleaf reported the number of new cases per week had dropped from around 100 at the peak of the epidemic to only eight.
President Sirleaf celebrated this news and, at the same time, framed the CHW program as part of the national fight against Ebola, setting an ambitious timeline to have the program functional within the next two to three years.
“We are going to make the final push to fight Ebola now, by supporting community workers to get the job done.”
President Ellen Johnson Sirleaf, at a U.S. Senate Foreign Relations Committee hearing (December 10, 2014)
In May 2015, as the last Ebola cases were being identified, the Ministry of Health convened representatives from 14 ministry departments, 13 of the country’s 15 County Health Teams, and 30 partner organizations to agree on a vision and road map for strengthening community health. They agreed on an action plan with two ambitious targets:
- Revise the existing Community Health Services Strategy and Plan to incorporate a vision for a professional, government-led CHW program in remote, rural areas by the end of 2015.
- Launch this new CHW program in January 2016.
Liberia came very close to meeting both deadlines.
By December 2015, a revised National Community Health Services Policy and Strategic Plan was adopted. The new plan was a turning point – it laid out a vision for a professional community health workforce to improve community-based service delivery in rural areas. This cohort would “provide preventive and curative health services to the most under-served communities, rebuild trust in the health system, enhance linkages to health facility services and create social stability and economic impact in vulnerable communities.”
The new CHW program (called the National Community Health Assistant Program in Liberia) was officially launched in July 2016.
President Sirleaf pushed to expedite implementation further with the goal of deploying 1,000 CHWs before she left office in January 2018. In fact by the end of her term, more than 2,000 CHWs had been recruited, trained, and deployed.
Detailed financial planning
During the early planning phase, long before program launch, Liberia developed detailed financial costing and sustainability modeling that helped the government track and study three key variables: potential costs, potential benefits, and potential funding. With these tools, Liberia could understand, at an extremely granular level, the costs and benefits of various elements of the program, as well as who might be willing to pay for them, and for how long. In addition, the government was able to identify financial gaps, both geographically and programmatically, match them with potential funders, and advocate for line-item resources, prioritizing specific items and geographic settings for further investments.
Liberia’s costing projections helped the Ministry of Health appear credible in its ongoing negotiations with donors and partners. For example, an analysis revealed the program would be affordable and sustainable, as the total running costs of the national CHW program (covering 29 percent of the national population and 60 percent of the rural population) would add only five percent to the national health budget.
Liberia used these tools to develop tailor-made investment cases for each donor. Through this research, Liberia asserted itself as an attractive investment opportunity for donors, helping accelerate donor commitments.
Case for investment in the scale-up of the National Community Health Assistant (NHCA) program

Ministry of Health of Liberia. Analysis replicated in Liberia's Reproductive, Maternal, New-Born, Child, and Adolescent Health (RMNCAH) Investment Case for the Global Financing Facility
*This was a tool used in financial planning and does not reflect observed data.
Liberia used its modeling tools to make convincing cases for support from diverse stakeholders. The below excerpt from a Ministry of Health presentation makes the case that the CHW program will not only have substantial health impacts, but will also create jobs and provide a nearly five-to-one ratio return on investment. Similarly, the Ministry of Health used these tools to translate the costed CHW program plan into Liberia’s Reproductive, Maternal, Newborn, Child, and Adolescent Health Investment Case for the Global Financing Facility, which resulted in a $5 million investment in the program.
These tools could also model different implementation strategies and programmatic options. For example, Liberia initially considered having two cadres of supervisors for its CHWs, one clinical supervisor and one peer supervisor who supported logistic, community engagements, and additional supervision. Evidence from the CHW pilot programs in Liberia and other countries (e.g., Bangladesh, Ethiopia, Benin, and India) were costed as potential options. This exercise helped the government understand the financial implications of a second supervisory cadre and led officials to move forward with a program that incorporates just one supervisor for each CHW.
*This was a tool used in financial planning and does not reflect observed data.
These costing tools enabled Liberia to take a more proactive stance with donors. It mapped what donors could bring to the table, illuminated ways to work around the restrictions that came along with that funding, and helped model ways to ensure coverage of the most critical expenses.
Donor management
With financial planning tools in place, Liberia did not have to accept what was offered, but instead could respond to funders’ offers with proposals that would maximize impact and demonstrate the need for investments to fill the critical gaps. As a result of such advocacy, the U.S. Agency for International Development (USAID) reprogrammed its Partnership for Advancing Community Based Services award in 2015 to fund the CHW program in three counties, and support training for supervisors in three others. The World Bank (initially via UNICEF) agreed to fund community health programming in five counties in the southeast (and later two more counties). Other donors and partners made similar adjustments.
As Liberia tracked and mapped each donor’s priorities, the country pushed less transparent donors to become more forthcoming about their own funding requirements. Liberia pushed for this information and captured it in their resource mapping tool to gain a more nuanced understanding of the funding puzzle that it leveraged to great effect. By identifying and navigating funders’ guardrails, Liberia mobilized a patchwork of highly restrictive funding to support a robust national CHW program.
As of 2019, almost every major health sector development donor is funding some aspect of Liberia’s CHW program. And while the funding map looks like a jigsaw puzzle (see below), the program implementation is meant to be uniform and seamless across counties, unaffected by the varied funding sources. For example, in Lofa County, the CHW program is supported by the Global Fund in some districts, and USAID in other districts, but they are meant to be no different from each other. Beyond the financial tools, the government used sets of standards, protocols, monitoring frameworks, data collection, and governance mechanisms to enforce this integration. In reality, achieving standardized implementation, regardless of funding, has proved difficult. (For more information, see section.)
CHW (Community Health Assistant) program implementation funding

As Liberia saw early success with its approach to funding, it was empowered to pressure donors to align their funding with the country’s plan and vision.
Funding availability by county (estimated in 2017)

*This was a tool used in financial planning and does not reflect observed data.
Data, measurement, and evaluation
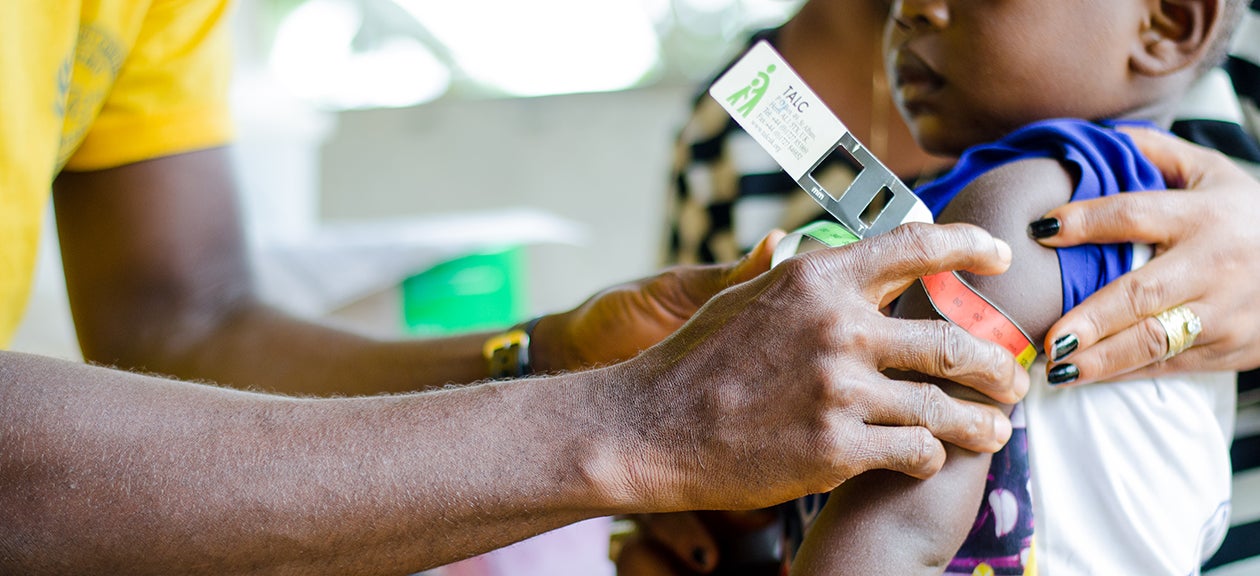
Data, measurement, and evaluation are central to the implementation of Liberia’s CHW program. The Ministry of Health collects data from a few key sources to identify and measure gaps, and monitor and improve implementation fidelity, program impact, and performance by CHWs individually, and by geographic setting. Data collection began in 2017, shortly after the first CHWs began working in the field.
The data can be roughly divided into three streams. One stream consists of routine data that originates from CHWs in the field and is focused on service delivery and disease monitoring. The second stream of data is from community-level and facility-level surveys that assess systems performance issues like supervision, supply chain issues, CHW competency, and financial audits. The third stream of data is from evaluations and other one-off research, like surveys of CHW and community perceptions, or impact evaluations.
Data collection by CHWs
The Ministry of Health gathers granular information about service delivery, drug usage, patient referrals, illnesses identified, and households served from CHWs.
Through the national community-based information system (CBIS), the Ministry of Health is able to track CHW performance and monitor outputs of the program via data entry into the national community-based information system (CBIS). The CBIS is integrated with the Ministry of Health’s broader health management information system, which tracks health care activities and monitors the burden of disease across the public sector health system. This integration connects Liberia’s last-mile health care system to the traditional health care system and enables them to formally “talk” to each other, facilitating the integrated management of primary health care.
CHWs monthly treatments of iCCM and malnutrition screenings

National Community Health Assistant Program Monthly Service Reports
Supervisors aggregate the data collected by CHWs into monthly reports for their health facility catchment area. The monthly reports are then digitized by county data entry clerks and entered into the CBIS. The chart below illustrates all data sets collected by CHWs and their supervisors, that are then entered into the CBIS. In addition to CBIS, CHWs identify disease triggers at the community level and feed this data into the disease surveillance system. This surveillance system is used to identify and respond to potential infectious disease risks across Liberia’s remote communities, a key goal of the CHW program.
Data sets collected by community health workers (CHAs) and their supervisors (CHSSs)

Beyond using data to measure performance, data at the district and county levels is also used to inform the allocation of additional resources and the timing of education campaigns. For example, spikes in the number of cases of diarrheal diseases might prompt local health officials to prioritize educational campaigns on water, sanitation, and hygiene issues.
From program launch, Liberia designed its data collection efforts to function in rural and remote areas. The data collection system was primarily paper-based, reflecting the lack of internet access and mobile phone coverage in remote areas.
Currently, some counties are piloting digitized CBIS data entry systems, in which CHWs use smartphone-based applications instead of paper forms. Digital systems can reduce the time required to collect and collate data and reduce the errors that occur when paper forms are digitized.
The digital data collection systems rely on phones or tablets that can also be used for CHW refresher trainings, field assessments, and to improve communication between CHWs and supervisors. These digital tools can make re-trainings and refresher courses easier to access, ensuring uniformity. However, digital tools can be a challenge for remote area CHWs, who often have little education and experience with digital devices.
The Ministry of Health is discussing standardizing the approach to data collection and continuing education for CHWs, using smartphones. Thus far, digital refresher trainings have been implemented unevenly, partly due to the availability of funding.
Data from facility and community surveys
The second stream of data is from the Implementation Fidelity Initiative – a set of facility and community surveys that help assess how closely program implementation aligns with the CHA national policy. These assessments help inform national discussions regarding program revisions to policies, tools, and processes, and arm the central MOH with data to address gaps in implementation. Improving data quality remains a priority for this national data set.
Among many other indicators, the surveys track four that are key to assessing program performance.
- Percentage of community health workers demonstrating curriculum knowledge
- Percentage of community health workers with all essential medical supplies in stock
- Percentage of community health workers who have received a supervisory visit from a nurse supervisor in the prior month
- Percentage of community health workers who have received their salaries on time
Representatives from the Community Health Services Division, the Health Monitoring, Evaluation, and Research Division of the Ministry of Health, and other staff conduct surveys measuring these indicators during quarterly field visits to counties. Additionally, representatives from the County Health Team also collect data monthly. (See below for selected questions IFI assesses.)
KEY QUESTIONS ADDRESSED BY THE IMPLEMENTATION FIDELITY INITIATIVE
Program includes Community Health Assistants (CHAs) and Community Health Services Supervisors (CHSSs)
| Recruitment | Training and Skills | Supply Chain | Supervision | Incentives | Service Delivery Quality |
|---|---|---|---|---|---|
Was the CHA recruited from the community he/she serves? | Are CHAs trained in all four modules of training? | Is the CHA in stock with life-saving commodities (ACT 25, ACT 50, amoxicillin, oral rehydration salts, zinc)? | Are CHAs receiving one or more visits from supervisor in the preceding month? | Are CHAs receiving correct monetary incentive amounts? | Have CHAs been routinely visiting households? |
How many CHAs are in this community? | Is the CHA equipped with their job aids and data forms, and filling out forms correctly? | Are CHA commodities in stock and appropriately stored at the facility level? | Do CHAs feel supported by supervisors? | Are CHAs receiving monetary incentive on time? | Are CHAs organizing health education and outreach at the community? |
How many CHSSs and CHAs are in the facility catchment area? | Are CHAs able to answer knowledge questions correctly? | Are supervisors providing feedback, reviewing forms, and checking on patient referrals? | Are supervisors spending appropriate time in facility and community? |
Data source for table: Last Mile Health
The Implementation Fidelity Initiative data, aggregated nationally and split by county, is reviewed by the Ministry of Health, County Health Teams, donors, and implementing partners at quarterly review meetings at the national and county levels. During these meetings, partners and officials identify performance gaps, share lessons, highlight successes, monitor long-term trends, and revise program designs in response to data and experience.
Following the review of data at quarterly review meetings, counties jointly determine action items and track them through a shared spreadsheet. At the central level, challenges relevant to all counties are tracked on one sheet and regional action points on subsequent sheets. These spreadsheets, which are available to County Health Teams and Ministry of Health staff involved in quarterly review meetings at the county and national levels, serve as an accountability mechanism to ensure change over time.
Data from evaluations and research
This data set draws from other evaluations, research, and studies designed to answer specific questions about program performance, impact, or design. For example, the “Program Perceptions” study helps assess perceptions of the program’s strengths and weaknesses via in-depth interviews with actors across Liberia’s community health system, including CHWs and community members, clinical supervisors, and officers in charge of health facilities where supervisors are based. The results of the analyses are presented back to stakeholders at national and county-level quarterly review meetings. Other studies include impact evaluations that assess the program’s contribution to health outcomes.
Governance structures
Liberia built multiple layers of new governance bodies to develop and manage its CHW program, each body with its own processes, agendas, meeting rhythms, and mandates. All key stakeholders, from the Ministry of Health to partners and community representatives, are required to participate in these groups to expedite and clarify decision-making. Each of these new governance bodies have different functions at the national, county, and local levels.
At the national level, the government established the Community Health Technical Working Group, which develops national policies for Liberia’s Revised National Community Health Services Policy and Strategic Plan, including CHW training curriculum and supervision. Within the working group, subgroups address the most common and critical challenges in the implementation and scale-up of a high-performing CHW program, such as supply chain improvements, monitoring and evaluation, training, recruitment, remuneration, and supervision. Every subgroup includes Ministry of Health personnel and representatives from donors and partners. Each subgroup reports the results of their research and deliberations back to the broader working group. These groups are organized around health systems functions and not vertical disease areas, and support alignment across MOH departments.
At the county level, County Health Teams perform quarterly reviews, which draw on data from CBIS and feedback from CHW supervisors to assess and improve performance. At the district level, District Health Officers ensure coordination, collaboration, and supervision of community health officers. At the facility level, Health Facility Development Committees (HFDC) are responsible for mobilizing and coordinating community health efforts within their catchment areas. The HFDCs also oversee the Community Health Committees within their catchment areas.
At the local level, Liberia leveraged existing community health committees, a diverse group of five to nine elected community volunteers, to support recruitment of CHWs, help coordinate and support their work, support referrals to facilities, promote the prevention of disease, and manage community sanitation and water supplies. The committees report to the nearest health facility.
The table below includes only a selection of governance structures established by Liberia.
PURPOSE OF TOP COMMITTEES AND OTHER KEY GOVERNANCE STRUCTURES
| COORDINATION FORUM | ROLE |
|---|---|
National—Community Health Technical Working Group | Supports CHWs and others to share information, align on implementation activities, support program design choices, and make decisions about resource allocation. The Community Health Technical Working Group has overseen the establishment and scale-up of the CHW program and will continue to operate under the new administration elected in 2018. Last Mile Health is secretariat of this group. |
National—Quarterly Review Meetings | Implementers and MOH gather to review progress, identify challenges, and joint problem-solve on implementation. |
County—Health Partner, Program Review Meetings | Regular coordination meetings at county level to coordinate NGO-supported activities and oversee progress of all county health sector activities. |
National Health Sector Coordination Committee | Strategy and coordination of overall MOH and health sector activities, including CHA Program. Last Mile Health is NGO representative of this group. |
National Annual National Health Policy Conference | Annual presentation of progress and strategy of all health sector initiatives. |
National President’s Delivery Unit | Tracks progress and provides broad-based political influence support for key presidential projects. CHA Program was one such project in previous administration - engagement with new PDU likely. |
Data source for table: Last Mile Health
Leveraging partnerships
Liberia leveraged nongovernmental organizations (NGOs) to lead initial program implementation and management. This approach allowed Liberia to harness the capacity of its partners to leapfrog over some tricky early hurdles. In addition, leaning on partners for early implementation enabled the government to slowly take over program management— and ownership—as its capabilities strengthened.
In 2016, the government of Liberia reiterated its goal to eventually manage the program and shift away from a reliance on fragmented partner implementation. The model, as illustrated below, allows international NGOs to rapidly ramp up execution and then slowly transition the management of the program to county health departments as government capacity increases.
This shift toward government management may improve sustainability, reduce costs (by cutting out the NGO "go-between"), and increase accountability. Moreover, local NGOs can provide ongoing capacity building support as needed. Currently, most counties are still transitioning to full government ownership of the program and are in phase two (see illustration below).
Four phases in transition of operational management of Liberia's CHA program to government

However, the government’s approach to gradually assume ownership also comes with important trade-offs. It remains unclear when certain counties will have the capacity to take over management, and the parallel management by partners has resulted in varying practices and poor implementation fidelity. For counties in phase three and four, there are ongoing assessments of quality and performance to determine whether further support is needed. (See section.)
Targeting
By implementing the CHW program only in communities that are at least five kilometers from a health center, the government achieved two critical goals:
- Reserved scarce resources for rural areas, where they were needed most. Disparities between urban and rural areas are significant in Liberia – for example, in the most recent Demographic and Health Survey in 2013, pregnant women in urban areas were more than twice as likely to have a skilled birth attendant during delivery than those in rural areas, and under-five mortality was 13.2 percent higher in rural areas.
- Bypassed opposition from groups invested in, and resistant to change within, established health systems, such as urban health care providers and partners supporting the early community health volunteer program that served almost exclusively peri-urban areas. That program has continued unchanged. Indeed, the CHW program did not directly replace any existing program. It simply filled a tremendous gap that had left about a third of Liberians without access to primary health care and the country vulnerable to unchecked epidemics. The program was seen as a win for communities and local governments who were provided, through the program, with unprecedented staff and resources.
The government’s targeting also led it to prioritize the program’s launch in the counties where it was needed most, based on surveys and disease burden.

Pilot before scaling
In 2012, Dr. Walter Gwenigale, then health minister, requested government partner Last Mile Health (then known as Tiyatien Health), to co-develop a pilot project to address shortcomings in the early community health volunteer program. Last Mile Health chose to establish the pilot in the Konobo district, Grand Gedeh County, where they were already working in partnership with the Ministry of Health. Compared to other districts, Konobo had worse maternal and child health outcomes than any other rural district.
The pilot included 54 CHWs and tested innovations that would later inform the new national CHW program to be launched in 2016. The CHWs were recruited from the communities where they lived and only remote communities (defined as those more than five kilometers from the nearest health facility) were targeted. The pilot training program contained four modules: community health and surveillance (added after Ebola), child health, maternal and neonatal health, and adult health. The child health module included integrated community case management protocols for community treatment and management of diarrhea, acute respiratory infection, and malaria, along with referral protocols for patients with clinical danger signs. These protocols were adapted from World Health Organization (WHO) guidelines. The CHWs received a monthly cash incentive of $60 for approximately 20 hours of work per week.
The key difference between the pilot and the national CHW program launched in 2016 was supervision, in addition to a small difference in pay. In the pilot project, CHWs had two supervisors: a community health worker “peer supervisor” that conducted weekly supervision visits to support logistics, community engagement, coaching, and a clinically trained “nurse supervisor,” that conducted monthly supervision visits. The national CHW program includes only one clinical supervisor.
Findings from the pilot showed significant improvements in access to health care for children suffering from diarrhea (up 60 percentage points), malaria (up 31 percentage points) and acute respiratory infection (up 51 percentage points). The rates of pregnant women undergoing clinic-based births with a skilled provider also increased, from 55 to 82 percent.
The WHO director general cited findings from the pilot in the Bulletin of the World Health Organization: “Enhanced recruitment, training, supervision, and compensation of community health workers rapidly improved coverage with maternal and child health services in rural areas of Liberia.” These results demonstrated that investments in a last-mile health system could pay off, if done in a targeted, disciplined way.
The pilot gave Liberia more than a model, it gave the country an advocacy tool.
Senior Ministry of Health leadership heard about successes and challenges directly from communities. Donors visited the pilot and were moved to support the program and mobilize additional resources. During the 2013 National Health Conference, Dr. Gwenigale profiled these results, inviting the County Health Team from Grand Gedeh and Last Mile Health to jointly present. He followed that presentation with the announcement that “this is the model we want to see in every village in the country.”
