Key Points
Liberia trained and fielded a cohort of nearly 4,000 well-trained, supervised, and paid CHWs to proactively provide a package of services that reflects the local disease burden and includes curative care.
Liberia’s CHW program reflected the WHO’s guidelines for CHW programs including integration into the formal health sector.
Liberia has long recognized its citizens’ poor access to primary health care and the potential role community health workers (CHWs; also called community health assistants or CHAs in Liberia) can play to help close this gap.
The government first launched CHW programming in the 2008 National Policy and Strategy on Community Health Services, which was further updated in 2011. At that time, only 51 doctors in Liberia served a population of roughly 3.7 million, more than one million of whom lived in remote areas more than five kilometers from a health facility staffed by trained medical professionals.
In 2008, only 51 doctors in Liberia served a population of roughly 3.7 million

To improve access to basic health care, Liberia approved a community health policy that called for a network of community health volunteers modeled after Nepal’s program of female community health volunteers. Fragmented policy implementation resulted in a patchwork of parallel programs launched by the government and nongovernmental partners as funding became available, with little standardized training, supervision, or services.
By 2013, community health volunteers numbered 8,052 and were divided among at least five volunteer cadres, from traditional midwives to community health promoters, each with distinct skills, training, services, incentives, and service areas. The variety proved more of a weakness than a strength. Research indicated that these cadres could not be relied upon, as a group, to consistently deliver a standardized package of high-quality primary health care services. Instead, there were gaps and overlapping services. The government was not positioned to address this problem because the various cadres of community health volunteers reported more often to nongovernmental organizations than to the government itself. Further, research found that volunteers were often poorly trained, unmotivated, and difficult to retain. Liberia’s health minister observed that because volunteers “were unpaid and under-supported, many dropped out or were ineffective in practice.” These challenges revealed the need for the more formal and integrated rural CHW program that followed.
The Ebola epidemic of 2014–2016 demonstrated the human cost of such a poorly functioning volunteer system. It also constrained access to health care in tangible ways, killing roughly 10 percent of Liberia’s doctors and eight percent of its nurses and midwives, or about eight percent of its total health workforce. Liberia’s health minister later observed that Liberia’s “lack of paid, well-supported CHWs helped fuel the spread of the 2014–2016 Ebola epidemic from rural communities into cities, claiming thousands of lives.”
In response, Liberia developed a new health sector investment plan, that included a new CHW program, the National Community Health Assistant Program. The CHA Program aimed to reach the most vulnerable communities in rural areas, with higher-quality services that better mirrored the local disease burden, would be monitored and managed by the government, and would be integrated into the formal health system. Launched in 2016, the CHA Program is, in many ways, the culmination of Liberia’s years of experience in community health.
The National Community Health Assistant Program positions CHWs as a paid, professionalized, and critical link between the most vulnerable communities and the national health system. The new CHW network was a significant change from the early community health volunteer program. The new cohort was trained in the delivery of a standardized set of integrated primary health services, supervised by front line clinicians such as nurses, deployed in sufficient numbers to reach every household in their catchment areas, regularly paid, and tasked with reliably collecting data for decision-making. Selected from the communities they serve, which are at least one-hour’s walk (or five kilometers) from the nearest health facility, CHWs deliver an integrated and standardized package of health services that includes curative and preventive care to the most vulnerable communities in the country. The cohort also functions as an early warning system against future infectious disease outbreaks.
Formally launched in 2016, the program, as of mid-2019, has trained and deployed 3,177 CHWs and 344 community health supervisors now working in 14 of Liberia’s 15 counties. By 2021, the program is expected to deploy 4,000 paid, professional CHWs and 400 clinical supervisors (mainly nurses based in community clinics). Each CHW is integrated into the national health system and provides a standardized package of essential life-saving services and epidemic surveillance within communities previously excluded from the national health system.
In addition to providing an integrated package of services, Liberia’s CHW program incorporates key features that ensure quality and standardization at scale, such as recruitment standards, national training, and remuneration requirements, management and supervision protocols, supply chain support, and robust monitoring and evaluation systems.
Package of services
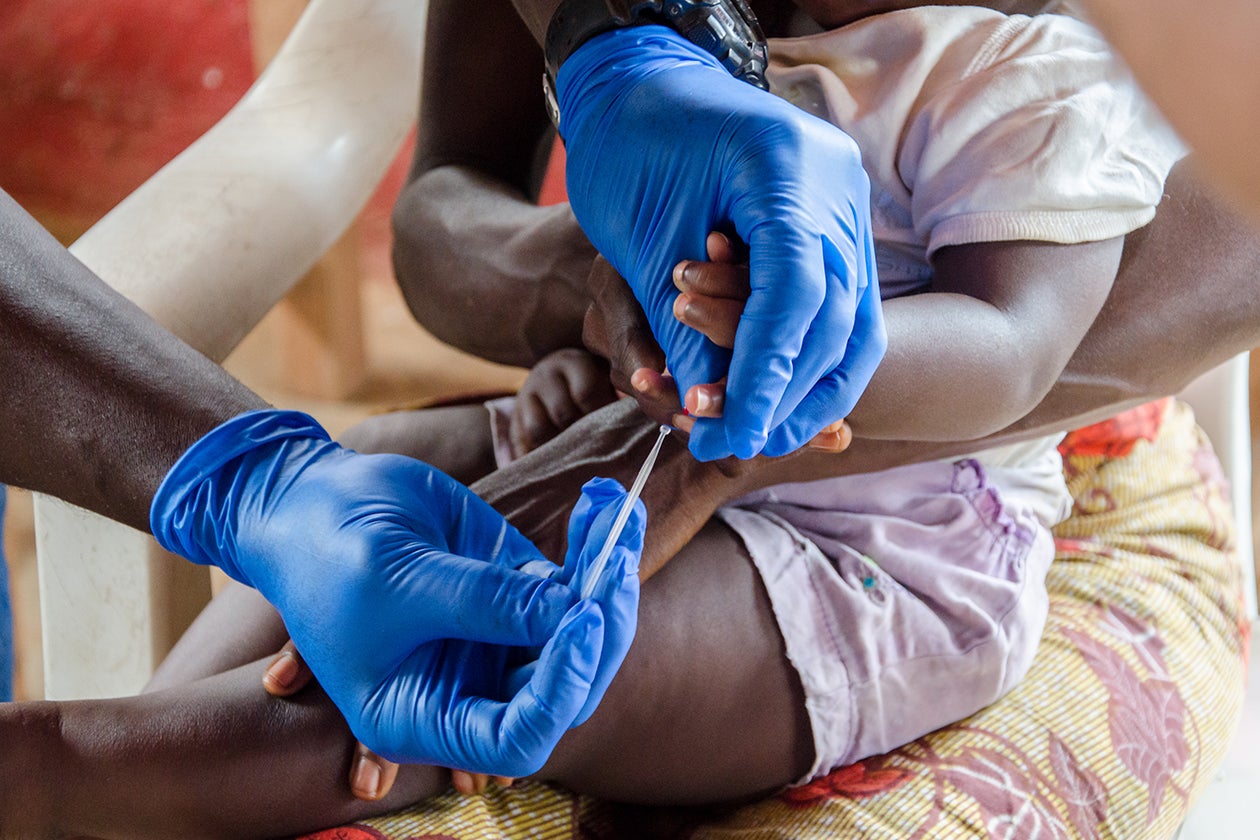
CHWs deliver an integrated and standardized package of primary health care services to a specific area that includes between 40 and 60 households (up to 350 people). In sparsely populated areas, the minimum number of households can be reduced to ensure each community has at least one CHA available. Regardless of the health status of household members, CHWs visit them at least once a month.
The services CHWs provide were selected to address the leading causes of morbidity and mortality in rural Liberia, based on data from a CHW pilot in Grand Gedeh County and the experience of early community health volunteer programs. The package of services also reflects current World Health Organization (WHO) prevention and treatment guidelines.
The package of health services that CHWs provide includes the following four key components (full list of services ):
- Robust community events-based surveillance for infectious diseases
- Reproductive, maternal, and neonatal health care, health promotion education, and distribution of family planning products, including oral contraceptives and condoms
- Integrated community case management of diarrhea, malaria, and acute respiratory infection in children under five, and screening and referral for malnutrition
- Adult health services including support for patients living with HIV, tuberculosis, and select neglected tropical diseases, as well as the provision of first aid and basic lifesaving skills for common emergencies
Integration with the formal health system
CHWs are recognized as a core component of the public sector health system and are formally integrated into the continuum of care. This means that patient referrals flow in both directions, from the CHW to the health facility, and from the health facility to the CHW. For example, a CHW may identify a pregnant woman who needs specialized care and refer her to a health facility. After treatment, the facility will likely refer the woman back to the same CHW for follow-up care. Such referrals are standard in more complex cases, such as children with severe cases of malnutrition or malaria, and in cases of leprosy, tuberculosis, or HIV. To ensure referrals to distant health facilities are feasible, CHW supervisors work with communities to identify available transport to and from health facilities.
CHWs are connected to the formal health system in other ways as well. They receive their supplies through the same supply chain network that serves health care facilities. CHWs also collect and share data with Liberia’s community-based information system, which is integrated into the national government’s health management information system. (For details on data collection and use, see Data, Measurement, and Evaluation section.)
Finally, CHW supervisors, based at the nearest health clinic, are a key link connecting CHWs to the formal health system.
CHW (National Community Health Assistant) program overview

Supervision
Liberia’s more than 3,000 CHWs are supervised by nearly 350 Community Health Services Supervisors (CHSS), clinically trained health staff such as nurses, midwives or physician assistants. Inspired by examples in Ghana and by Alaska’s Community Health Aide Program, Liberia made a deliberate decision to ensure these supervisors were clinically trained health workers, equipped to enhance the supervision of CHWs and strengthen the care provided in remote communities.
Supervisors provide clinical expertise and mentorship, restock supplies (see for more information on stocking challenges), and supervise as many as ten CHWs in their health facility’s catchment area. Supervisors spend at least 80 percent of their time in the field, visiting each CHW at least once a month - although this does not always occur. Supervisors are meant to provide CHW oversight four days a week in the communities they serve, and one day a week at the nearest health facility, which is often a community clinic or primary health center.
Supervisors receive four weeks of in-depth training on the integrated service delivery package delivered by CHWs, and practical training on the provision of supportive supervision, clinical mentorship, coaching for CHWs in the field, and support for the referral of patients who need more sophisticated care in the clinic. These trainings are conducted by master trainers who are trained at the national level. Supervisors report directly to the officer in charge of their health facility, which provides another layer of connection between the community health system and the facility-based health system.
Initially, the Ministry of Health explored supporting two types of supervisors for its CHWs – one clinical supervisor who meets with each CHW monthly to check on patient treatment and improve CHW skills, and one non-clinical operational supervisor, who meets with the CHW weekly, speaks the local language, counsels on community engagement, supports patient referrals to and from facilities, and helps the CHW plan and restock supplies as needed. This two-pronged supervisory structure was modeled on Liberia’s Grand Gedeh County CHW pilot program, in which every CHW had both a clinical supervisor and a peer supervisor. After consulting with technical experts and analyzing cost implications, however, Liberia determined that expanding labor costs to accommodate two cohorts of supervisors would jeopardize the program’s sustainability. Liberia therefore limited supervision to one cohort of highly skilled clinical supervisors, who are also tasked with providing logistical support. This tact emphasized clinical expertise and allowed for ongoing mentoring to supplement formal trainings.
CHW recruitment
Locally elected Community Health Committees are groups of five to nine local residents who oversee the recruitment and selection of CHWs from within their own community.
Committees aim to give preference to female candidates and those with prior experience engaging in health promotion work at the community level. The preference for individuals with past experience was intended to facilitate the transition of capable community health volunteers from the pre-existing community health system to the CHA Program. The preference for female candidates reflects multiple policy objectives, including improving reproductive, maternal, newborn, child, and adolescent health, economically empowering women and improving their representation in the health sector, and recruiting individuals in rural and remote areas who are less likely to have formal employment experience. Despite this preference for female candidates, hiring women to serve as CHWs has proved challenging. (See Challenges section for more on Liberia's difficulty hiring women CHWs, and its plans to overcome this hurdle.)
CHW candidates must meet the following qualifications:
- Be a permanent resident of the community they seek to serve
- Be between 18 and 50 years of age, and physically able to walk more than one hour to reach communities in their catchment area
- Have a minimum sixth-grade education
- Demonstrate basic literacy and numeracy skills in English, and fluency in relevant local dialect(s)
Training
Training programs for CHWs strike a balance between classroom lectures and practice in the field. Long trainings away from the community are minimized as they can pose multiple challenges, including discouraging participation of women, and interrupting existing service delivery.
The standard training protocols are organized as a series of four in-classroom training sessions or “modules” of approximately two weeks each. The modules, each of which are followed by four to eight weeks of practice in the field, focus on the components of Liberia’s tailored service delivery package (full list of services ):
- Community event-based surveillance
- Reproductive, maternal, and newborn health
- Child health
- Services for adults including HIV, tuberculosis, neglected tropical diseases, mental health, and first aid
CHW (National Community Health Assistant) training cascade

Liberia’s program relies on a training-of-trainer approach, also called a cascade approach, in which two community health service supervisors (CHSSs), with the support of two master trainers from the Ministry of Health and/or County Health Teams, train groups of roughly 25 CHWs. Trainings are organized and delivered at the district or county level. The master trainers also train groups of clinical supervisors.
Before each training module, CHWs take a pretest to evaluate their skills in the corresponding subject area. Following each training session, CHWs return to their communities for four to eight weeks to practice under supportive supervision. Before beginning the next module, they take a post-training, which involves a written exam and demonstration of skills (by providing care while a supervisor watches). If CHWs do not obtain satisfactory post-training scores, they are required to repeat training until they achieve a passing score. In that circumstance, they would typically receive remedial supervision in the field.
After completing training, CHWs are clinically supervised and receive drug supplies at least once per month. Supervision involves meeting with a supervisor to both discuss performance, opportunities for improvement, challenges, and the general health in the community, and have the supervisor observe the CHW’s performance. CHWs also collect data on the services they provide and share that data with their supervisors. That data enables County Health Teams, health facility development committees, and other local stakeholders to identify which CHWs might be underperforming, to target support to health workers most in need. (See more on .)
Remuneration

To encourage commitment and retention, CHWs are paid $70 per month, commensurate with the 20 hours of work they are expected to perform each week. Though CHWs are contracted by the national government and paid by County Health Teams, they are not considered civil servants. Clinically trained supervisors are usually paid $269 per month, though supervisors in particularly remote counties are paid up to $313 per month. Some CHSS (29 as of October 2019) are on government payroll as civil servants.
The remuneration of CHWs illustrates how Liberia held on to its vision for the program while making smaller compromises with donors. Several major donors did not support the designation of CHWs as civil servants, and some opposed paying them, especially donors that had been involved in the community health volunteer programs and were committed to that model. These donors were concerned about the sustainability of adding to the government’s already sizable workforce. Salaries for government employees totaled nearly 30 percent of public expenditures between 2010 and 2015, and made up nearly half of all formal employment in the country.
The government, however, was determined to pay CHWs, based on evidence from other countries and because of poor performance of earlier community health volunteers.
Liberian officials also understood that serving as a health worker is dangerous, given the national experience with Ebola. As a result, officials were sensitive to demands that health workers be paid in a manner that reflects the risks they take, as well as the value of their work. In July 2013, Liberian health workers went on strike over low pay and delays in payment, which further elevated the issue of adequate and timely pay for frontline health workers. (For more on the value the government placed on health professionals, see contextual factors in section.)
In response to continued pressure from donors to preserve a volunteer-based CHW model, the minister of health and president made several public statements in support of paying community health workers, signaling it was not up for negotiation. After debate among the Ministry of Health’s senior leadership team, the Community Health Service Division made a final recommendation to provide a $70 per month base incentive, with the compromise that CHWs would not be considered government employees. Their compensation would technically be an “incentive.” In fact, Liberia calls them “community health assistants” rather than “community health workers,” to reflect this compromise.
