Under-five mortality reduction in Ethiopia
From 2000 to 2015, Ethiopia’s under-five mortality rate decreased by 56 percent.
CONTENTS
Quick Downloads

Key Insights
Ethiopia clearly stands out as an exemplar of under-five mortality reduction, though challenges remain to continue making progress. That one of the world’s poorest countries could achieve this reduction across such a large and diverse population, and throughout a vast geographic area, makes it a promising model for a wide range of low- and middle-income countries in sub-Saharan Africa and beyond.
Ethiopia clearly stands out as an exemplar of under-five mortality reduction, though challenges remain to continue making progress. That one of the world’s poorest countries could achieve this reduction across such a large and diverse population, and throughout a vast geographic area, makes it a promising model for a wide range of low- and middle-income countries in sub-Saharan Africa and beyond.
Creating a strong, comprehensive community health system, centered on a highly successful Health Extension Program
The creation of the national Health Extension Program was fundamental to the establishment of an effective national community health system. Key informants repeatedly singled out the Health Extension Program as crucial to the country’s success in reducing U5M. One FMOH official referred to it as “the major umbrella” covering Ethiopia’s child health initiatives.
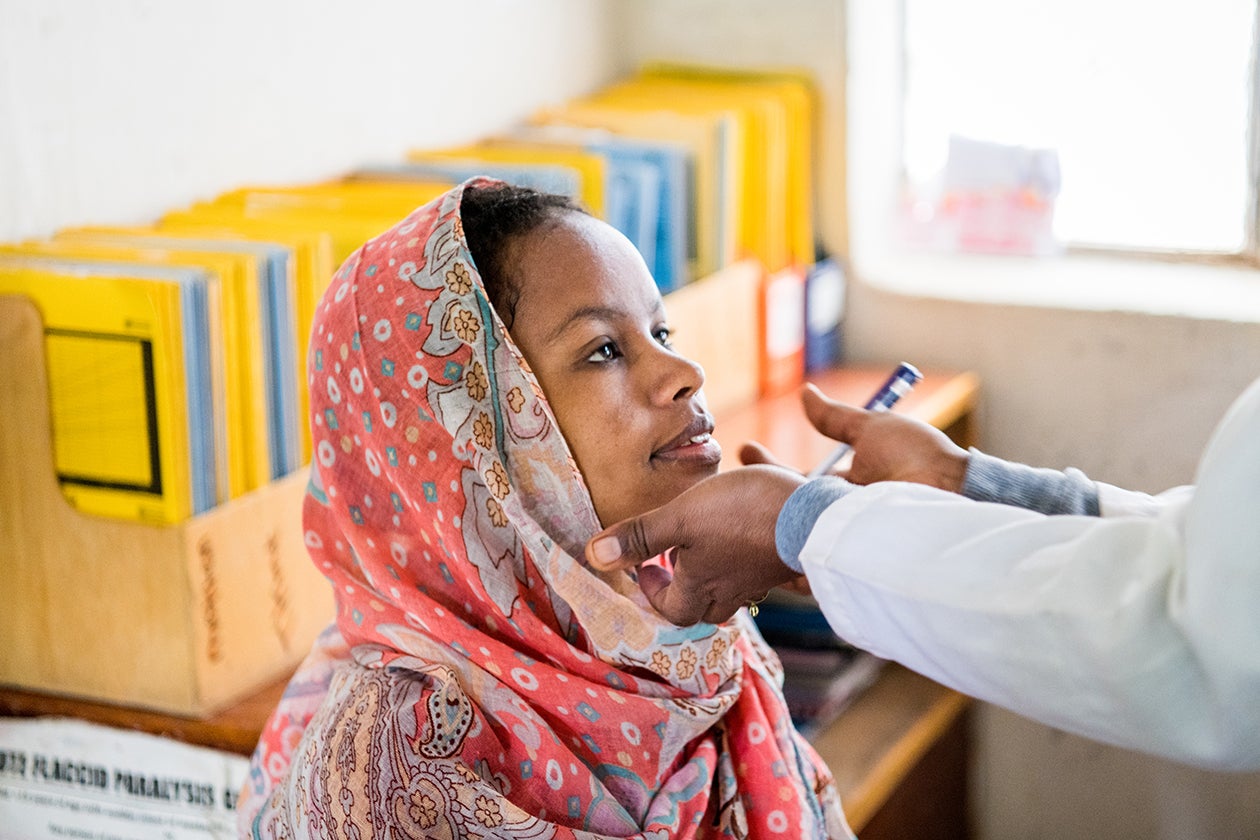
Health Extension Workers (HEWs) played an instrumental part in carrying out U5M interventions, making health services more accessible to many communities that previously had little or no access to them.
The Health Extension Program provided preventive services such as immunizations and distribution of insecticide-treated malaria bed nets. As it grew, it also offered curative services, particularly in rural areas. The Health Extension Program soon became a widespread national program that reached many rural and pastoralist areas traditionally underserved by static health facilities. It evolved into a platform for introducing new programs such as Integrated Community Case Management, and for delivering services typically provided in health centers and larger facilities, including immunizations and antenatal care.
Strengthening the national primary health care system and infrastructure
During the study period the government worked to advance the construction of health posts and health centers throughout the country, and to convert existing health centers to primary hospitals in order to increase access to comprehensive primary health care.
In addition to expanding facilities and infrastructure, Ethiopia’s ministries collaborated to strengthen the health workforce. The government implemented new training programs for physicians, midwives, and other health professionals—and improved programs that were already in place. It also created new cadres of health workers to alleviate the national health personnel shortage and increase access to care.

Commitment to data collection and use, pilot testing, and rapid scale-up of interventions
In its efforts to reduce U5M, Ethiopia made heavy use of data to assess disease burden and set priorities. This was often followed by small-scale implementation and pilot studies, followed by rapid national expansion.

Ethiopia has a long history of valuing data and using it for planning, prioritization, and implementation of new initiatives. Several national surveys are conducted in Ethiopia and have been used to guide policy and planning, including the Demographic Health Survey, Ethiopia Service Provision Assessment, Service Availability and Readiness Assessment, and Malaria Indicator Survey.
In addition to these surveys, the FMOH uses data from the Health Management Information System and local studies to inform many activities, such as setting national priorities, determining appropriateness of specific interventions, and planning the implementation of those interventions.
Availability of significant donor and partner resources, and the government’s ability to coordinate these resources effectively
Ethiopia’s campaign to reduce U5M benefited immensely from a strong influx of donor and partner resources over the study period. In addition to financial resources, donors and partners provided the FMOH with technical and human resources that advanced U5M interventions, often beginning in the exploration and preparation phases.
Coordination of these partners and their resources (whether financial or operational) was extremely important, and the government took it very seriously, adopting a “one plan, one budget, and one report” approach under which all parties involved in the health sector must align their activities with the priorities of the government. This allowed the ministry to guide resources efficiently, including the resources from international donors and partners. Rather than resulting in parallel programs, external resources in Ethiopia were leveraged to support government-led initiatives.


Under-five mortality reduction in Ethiopia

Ask an Expert
Our team and partners are available to answer questions that clarify our research, insights, methodology, and conclusions.
